Chronic stress can inflame the gut — now scientists know why
- NEWS
- 25 May 2023
Signals originating in the brain make their way to gut nerve cells, leading to a release of inflammatory chemicals.
By
- Saima Sidik
Search author on:PubMed Google Scholar
- [Email](mailto:?subject=Chronic stress can inflame the gut — now scientists know why&body=https%3A%2F%2Fwww.nature.com%2Farticles%2Fd41586-023-01700-y)
Access through your institution
Psychological stress is known to worsen the gut inflammation caused by certain bowel diseases. Now scientists have found out why. New research1 outlines a sweeping narrative that begins with chemical cues produced in the brain and ends with immune cells in the gut — a sequence that spells trouble for people with these conditions.
Access options
Access through your institution
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
27,99 € / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
199,00 € per year
only 3,90 € per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Additional access options:
Nature 618, 221-222 (2023)
doi: https://doi.org/10.1038/d41586-023-01700-y
References
- Schneider, K. M. et al. Cell https://doi.org/10.1016/j.cell.2023.05.001 (2023).
Related Articles
[
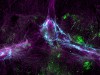
Guardians of the brain: how a special immune system protects our grey matter](https://www.nature.com/articles/d41586-022-01502-8)[

Gut feeling yields evidence of microbial involvement in autoimmunity](https://www.nature.com/articles/d41586-021-01837-8)[

Your brain could be controlling how sick you get — and how you recover](https://www.nature.com/articles/d41586-023-00509-z)[
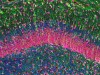
Brain-cell growth keeps mood disorders at bay](https://www.nature.com/articles/d41586-022-02210-z)
Subjects
Latest on:
[Architecture, dynamics and biogenesis of GluA3 AMPA glutamate receptors
Article01 JUL 25](https://www.nature.com/articles/s41586-025-09325-z)[\
‘Place’ neurons recognize the same spot from close by and far away
News & Views01 JUL 25](https://www.nature.com/articles/d41586-025-01716-6)[\
How fast are you ageing? Ordinary brain scans reveal the pace
News01 JUL 25](https://www.nature.com/articles/d41586-025-02086-9)
[
Ageing is linked to inflammation — but only in the industrialized world
News30 JUN 25](https://www.nature.com/articles/d41586-025-02085-w)[\
RFK Jr’s vaccine advisers vote down flu-shot ingredient — but back some jabs
News26 JUN 25](https://www.nature.com/articles/d41586-025-02000-3)[\
Rescuing dendritic cell interstitial motility sustains antitumour immunity
Article25 JUN 25](https://www.nature.com/articles/s41586-025-09202-9)
[
‘Place’ neurons recognize the same spot from close by and far away
News & Views01 JUL 25](https://www.nature.com/articles/d41586-025-01716-6)[\
How fast are you ageing? Ordinary brain scans reveal the pace
News01 JUL 25](https://www.nature.com/articles/d41586-025-02086-9)[\
Eureka! The brain science behind lightbulb moments
News Feature25 JUN 25](https://www.nature.com/articles/d41586-025-01963-7)
Jobs
6 major schools are now hiring faculty members.
Shanghai, China
ShanghaiTech University
Join theMax Perutz Labs as Full Professor to unravel disease mechanisms—from metabolism and stress to RNA regulation, epigenetics, and immunity.
Vienna BioCenter, Austria
Max Perutz Labs, University of Vienna
The Jena University Hospital (JUH) invites applications for a Professorship for Dental Prosthetics and Materials Science (W3) to be filled at the e...
07743, Zentrum (DE)
Friedrich-Schiller-Universität Jena
Tenure-track / Tenured Faculty and Young Outstanding Scholar Program Postdoctoral Research Fellows.
No.16, TianRong Street, Daxing District, Beijing
National Institute of Pathogen Biology, CAMS&PUMC
IFReC, The University of Osaka in Japan offers Advanced Postdoc Positions for Immunology, Cell Biology, Bioinformatics and Bioimaging.
Suita Campus, The University of Osaka in Osaka, Japan
Immunology Frontier Research Center, The University of Osaka

